Gabriela Gutiérrez, Argentina has been granted the TTS Scientific Congress Award

Adherence and medical outcomes, in adolescents/young adults following pediatric kidney transplantation: a transition experience between two public tertiary hospitals in Argentina
Marta L Monteverde1, Julieta Raño2, Gabriela Gutiérrez1, Natalia Robledo1, Juan Ibáñez1, Alicia Chaparro1, Rubén Schiavelli 2.
1Renal Transplant Unit - Nephrology, Hospital Prof. Dr. Juan P. Garrahan, Buenos Aires, Argentina; 2Deparment of Nephrology, Hospital Dr Cosme Argerich, Buenos Aires, Argentina
Introduction: Transition from pediatric to adult care is a critical time, with highest rates of rejection, death with a functioning graft, and graft loss due to non-adherence to immunosuppression
The aim of this study was to evaluate in kidney transplant pediatric recipients transplanted and followed-up at a public referral center the impact of transition from pediatric to adult health care on medical outcomes and measures of adherence
Methods: We followed the course of patients who received a Kidney Transplant at Hospital Garrahan and were subsequently transitioned to an adult public hospital (2002-2022). Data were collected from the SINTRA public registry, and from Hospital Garrahan’s, (pediatric) and Argerich’s (adult provider) electronic clinical records
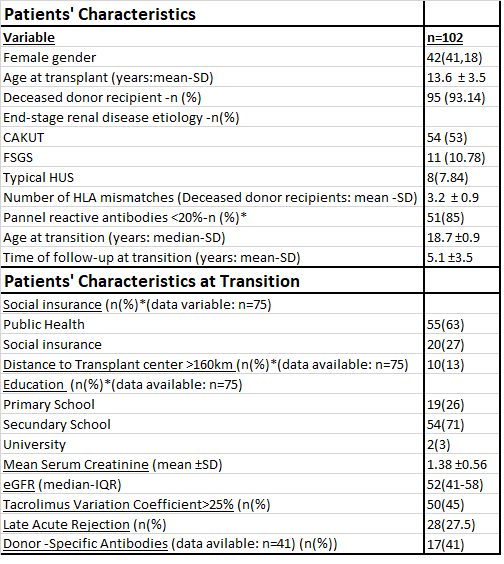
Results: We included 102 patients, 42% females, with a mean age at transplant of 13.6 years; 95% of them received a deceased donor graft. Main cause of CKD was CAKUT (53%). Mean age at transition was 18.7 y. Mean time of follow up at transition was 5.1 years. At time of transition, 45% had a tacrolimus Coefficient Variation (CV) >25%. (Table 1). Median time of follow-up from transplant time was 8.8 years; (IQR: 6-13) and from transition 3.6y (IQR: 1.9-6.5). Patient and graft survival at 10 years post-transplant were 97% and 75% respectively. Thirty-six (35%) grafts were lost, 47% in the first 3 years post transition.
Dividing the cohort according to transplant time in 2 eras: era1 from 2002 to 2015, and era 2, from 2016-2022, graft loss rate after transition decreased from 42.7% (n=32/75) to 14.8% (n=4/27); p=0.009. Main cause of graft loss was rejection (n=30; 83%). Those with a TAC coefficient variation ≥ 25% had higher risk of graft loss (HR: 6.25; CI 95%:1.38 - 28.26), p=0.0017). Three patients died (era 1), 2 with a functioning graft; 2/3 had comorbid- psychiatric illness.
Conclusion: Our findings suggest that time at transition is a period of increased vulnerability for this cohort of pediatric patients, with worse health outcome and decreased adherence. As the approach to transition by both, pediatric and adult teams become stronger, graft loss decreases. It is imperative to identify those adolescents with the highest risk of graft loss
[1] M. A. Chisholm-Burns /American Journal of Transplantation 2009; 9: 2497–2504
[2] Fredericks EM/ Pediatr Transplantation 2010: 14: 944–953
[3] L Pape/ Pediatr Transplantation 2013: 17: 518–524